Educational Highlights
With the full commitment of our Sutter Health Family Medicine faculty and academic team, Residents will have the opportunity to provide patient-centered team-based care for Northern California's diverse communities. Our exciting collaborations across departments, institutions, and participating teaching sites will provide innovative training that will prepare you for the future of family medicine.
Education and Community Involvement
Women's Health
Our residents enjoy a high quality and comprehensive women's and reproductive health education. Why refer patients out for services we can provide in a familiar and comfortable medical home? Under the guidance of core faculty who specialize in reproductive health, our residents integrate wide-ranging women's health procedures into their own continuity clinics and participate in dedicated procedural clinics.

During residency, interested trainees can gain competency in medical and surgical TABs, miscarriage management, gynecological ultrasound, colposcopies and cervical biopsies, endometrial biopsies, and IUD and Nexplanon insertions. We not only diagnose cervical dysplasia and cancer, but also provide treatment with LEEPs and cryotherapy.
Here at the Sutter Family Medicine Residency program, we offer a wide variety of educational experiences in obstetrical and maternity care. Our goal is to provide residents with a positive OB experience and graduate family medicine doctors who are competent and confident to take care of a broad array of OB patients. Our residents care for their own continuity patients in the clinic and deliver alongside our family medicine faculty as well as community OB/GYNs.
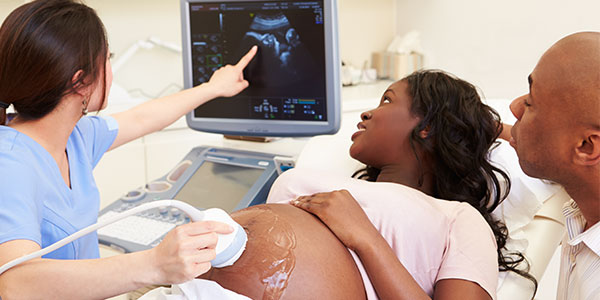
Additionally, residents interested in more advanced OB education have the opportunity to manage high-risk and diabetic patients in our clinic and manage patients undergoing a trial of labor after cesarean section. Residents may also take part in cesarean sections with our OB/GYN colleagues as well as Dr. Ryan Spielvogel and Dr. Megan Ash, family medicine faculty who perform cesarean sections.
After delivery, we continue to provide comprehensive care to both mother and baby. We promote postpartum contraception and family planning. We strongly encourage breastfeeding among our new mothers and are proud to boast that both Sutter Medical Center Sacramento and Sutter Davis Hospital have been designated a baby-friendly hospitals. Our residents do home visits for new mothers with social challenges.
Best of all, we often become the doctors of the babies we deliver!
Office-based and point-of-care ultrasound is starting to overshadow traditional diagnostic tools like the stethoscope and tongue depressor. We are on the cutting edge of this technology with high-end ultrasound machines in our clinics and handheld V-Scan devices.
Residents are trained in using ultrasound for not just prenatal purposes, but for IUD placement, abnormal vaginal bleeding, biliary disease, aortic aneurysm, hydronephrosis, vascular imaging, differentiation of cysts/masses/abscesses, and for musculoskeletal imaging including joint aspiration/injection. Images can be uploaded into patient records and archived for teaching purposes. Our residents and their spouses’ own pregnancies never lack for ultrasound pictures!
Multiple online training resources are available as well, including Sonosite’s website and through the University of South Carolina. We also have extensive teaching aids through the American Institute of Ultrasound in Medicine (AIUM).
Orthopedic Health
Sports Medicine provides advanced care not just for athletes, but for anyone who enjoys physical activity. It can help your patient get back to the top of their game or simply back to the active life that they enjoy.
Sports medicine primary care physicians help their patients improve performance, enhance overall health, prevent injury and maintain their physical activity throughout their lives.
At the Sutter Health Family Medicine Residency Program, family physician Paiyuam Asnaashari, D.O. (“Dr. Pai”), board certified in Sports Medicine, enjoys teaching musculoskeletal assessment – including POCUS evaluation – and management of common and uncommon MSK injuries.
Goals of our Sports Medicine training include:
- Diagnosis and treatment of sports or activity-related injuries and illnesses.
- Use of manual techniques to prevent and treat musculoskeletal conditions common in athletes.
- Special knowledge of the principles of athletic conditioning.
- Focus on injury prevention and rehabilitation, including injuries common to specific sports.
- Nutritional guidance to build strength and endurance in support of athletic perform.

In addition to traditional allopathic medicine, our residency offers education in Osteopathic Manipulative Medicine. Both M.D. and D.O. residents will be educated on common musculoskeletal complaints, and how to use their hands to diagnose and help alleviate common conditions like back pain in pregnancy and tension headaches. Taught by a board-certified Neuromusculoskeletal Medicine physician Jeffrey Brodovsky, D.O., residents will gain valuable skills in manual medicine.
Mental Health
We view Substance Use Disorder intervention as a core competency of any family physician. Our residency incorporates substance misuse (eg. alcohol, tobacco, opiates, stimulants) in the longitudinal Human Behavior and Mental Health curriculum, as well as during the PGY1 Psychiatry rotation and PGY2 Addiction Medicine rotation. During continuity clinic and inpatient rounds; residents gain experience in substance use disorder screening, intervention, and treatment. Our core physician faculty have x-waiver licenses and residents gain Suboxone training during continuum. We also have core faculty in the Motivational Interviewing (MI) Network of Trainers, who helps residents gain competency in this brief intervention.
Assisting patients with mental health issues, substance misuse, and behavior change are key elements in our family medicine clinics. To fully integrate the biopsychosocial model, our full-time behavioral scientist regularly precepts with physician faculty during continuity clinic and inpatient rounds. This enables ongoing, real time feedback about doctor-patient communication, contextual factors, psychosocial issues, and mental health disorders. We strive to apply evidence-based practices for integrative care within our continuity clinics utilizing an interdisciplinary team and community referrals. Residents can also opt to use elective time for additional experiences in areas such as Addiction Medicine, Psychotherapy, Chronic Pain, Corrections Medicine, Lifestyle & Self-Management strategies, Spirituality in Medicine, and Well-being.
Other Education
Celebrating diversity and encouraging all to be their most genuine selves is at the heart of our residency. We bring this philosophy with us when providing care to the transgender community — a traditionally marginalized patient population whose attempted suicide rates near 50%. Residents have the option to take a dedicated elective in transgender medicine offered in our clinic in conjunction with the Gender Health Center, a local non-profit aimed at serving the transgender community. Through the elective, residents become proficient in hormone initiation and management, develop an understanding of ancillary community resources, and will also learn how to navigate the often treacherous psychosocial waters that these patients must sail.
At its core, a Family Physician aims to relieve suffering. In June of 2016, California became the fifth state to legalize medical aid in dying. Through the End-of-Life Option Act, physicians are allowed to prescribe lethal medications to patients suffering at the end of their lives. In their second and third years, participating residents will have the opportunity to manage medical aid in dying in our clinic. Whether through in-office visits, telemedicine visits or home visits, residents help guide patients and their families through trying times and final hours with the utmost compassion and humanity.
We are proud of the communities we serve and the broad spectrum of care we can provide to our patients. As such, we are lucky to have on staff Dr. Greer — an American Academy of HIV Medicine certified HIV specialist. Through electives on HIV medicine and the mentorship of Dr. Greer, interested residents can become proficient in initiating and managing antiretrovirals, as well as managing complications from HIV/AIDS. Dedicated residents can also become eligible to sit for their certification exams and become certified HIV specialists themselves. We are honored to be training the next generation of providers for this underserved patient population.
Our program encourages residents to enhance appreciation and understanding of Integrative Medicine through mind, body, and spirit. Residents have the option to work with Sutter clinicians focusing in this approach (in both Sacramento and San Francisco), complete online courses, and/or attend a longitudinal or away elective such as the University of Arizona Integrative Medicine Rotation.

Residency is hard. Our program knows Physicians are likely to develop many of their wellness patterns during residency just as they develop other behaviors that are part of medicine. These 3 years are the ideal time to facilitate development of well-being practices to have career long impact. Therefore, we integrate wellness throughout the residency experience.

Residents enjoy having 2-week rotation blocks, jeopardy call, representation at faculty meetings; as well as easy parking and food at the physician lounge. We regularly offer support groups, Balint, cohort retreats, program retreat, wellness activities (such as yoga, qi gong), team building (eg. Volunteer at foodbank, float down the American River), and administrative support (eg. ‘Friend with EPIC’/EHR, quality improvement of clinic operations). Our behavioral scientist is available at all times; as are senior residents, faculty advisors, and employee assistance program (EAP). There is also a Well-being elective to provide protected time for the resident to focus on creating a sustainable wellness plan for themselves and to model for patients.
Scholarly Activities and Research
We dedicate time and resources to promote research and scholarly activity among both Resident and Faculty Physicians. During didactics, residents present journal club articles, as well as teaching a core Family Medicine topic. Sutter Medical Center library personnel are available to assist with research and scholarly activities, as well as the staff at SIMR, the Sutter Institute for Medical Research. Specific didactics are provided each year to introduce these resources to residents. In addition, residents may choose to participate in research studies and scholarly articles that residency faculty are undertaking.

Some recent projects include:
-
- Preconception CoIIN project– Investigate and innovate new approaches to pregnancy intention screening and follow up delivery in primary care setting
- The PATHFINDER study– A prospective study of 6,200 participants using the Grail multi-cancer blood test for screening and identification of multiple cancer types
- ROSES– A 3-year implementation study of ROSES, an evidence-based intervention to prevent postpartum depression in low-income women.
- Behavioral Health Integration (BHI) Project – Our Sacramento track received a large 2-year grant from DHCS to improve physical and behavioral health outcomes, care delivery efficiency, and patient experience by establishing fully integrated behavioral health care in continuity clinic (particularly for our patients with Medi-Cal). Faculty, residents & staff collaborate to establish this program and track outcomes including healthcare access, population health metrics, patient improvement, and physician satisfaction.
- Medication Assisted Treatment (MAT) for SUD Project – Both our Sacramento & Davis tracks received 1-year grants from CAFP to improve integration of MAT in our continuity clinics. Our faculty, residents & staff work together to adjust clinic workflows to address substance use disorders in our patients, increase engagement, lower barriers to care, and improve patient outcomes.
- Interpersonal Violence Prevention (IPV)– Qualitative research exploring the impact of California’s physician IPV mandated reporting law.
-
Community Involvement
Community medicine is an inherent part of Family Medicine. Sacramento is one of the most diverse cities in the nation. As both a college town and agricultural hub, Davis also represents a wide range of cultures. Our continuity clinics and hospitals fully reflect the communities in which we practice. Our residents get robust experience working with patients of various languages, ethnicities, religions, sexual identities, socioeconomic statuses, gender identities, nationalities, indigenous heritages, and ages. In this way, community medicine is embedded within our continuity clinics. Our clinics are the foundational home of our training program. Residents spend an increasing amount of time within clinic during all three years, with direct observation, feedback, and guidance available at all times. All of our core physician faculty also have their own continuity clinic within the residency program clinics. This ensures a true primary care clinic experience for residents and mentorship by practicing physicians. Our primary care clinics are staffed with medical assistants, social workers, pharmacists, nurses, and health care coordinators to assure an integrated team approach.
In addition, we actively cultivate community partnerships as a residency and intentionally include resident training beyond our hospital and clinic walls. Some of our partners and collaborators are:
- Wellspace
- Communicare
- One Community Health
- Gender Health Center
- Transitions
- Grant High School Sports Physicals
- Sacramento County Primary Health
- California Department of Corrections & Rehabilitation
- VA Northern California Health Care System
- La Familia
- Planned Parenthood
- Joshua House
- Building Healthy Communities
- Transformative Justice in Education
- Global Health: In past few years residents & faculty have gone to Tanzania, Ethiopia, India, and Thailand
The Future Faces of Family Medicine project is a mentoring program set up by Sutter Health and UC Davis Family Medicine residents to inspire local high school students to become primary care physicians. The program has received statewide and nationwide attention. This video was produced with the help of the California Academy of Family Physicians (CAFP).
Located in the capital of California, we have strategic proximity to our legislators, media hubs, and community initiatives. Our faculty and residents are active in the community and there are opportunities to get involved in local, state, and national efforts. Dr. Hitzeman was former editor and district board member at CAFP and encourages the entire FMRP community to participate in their Annual Advocacy Day. Dr. Spielvogel has provided testimony at the State Capitol on multiple occasions regarding the End-of-Life Options Act (ELOA),and is a founding member of the ACAMAID (American Clinicians Academy on Medical Aid in Dying) national medical society. In 2021, he authored a CAFP resolution to extend ELOA legislation and support removal of the 15-day waiting period. Dr. Brothers and resident physicians Tiffany Chen and Taylor Duke presented and subsequently received official approval for a CAFP resolution to eliminate barriers to same-day billing for primary care and mental health services. Drs. Brothers & Kettle work to ensure our Health Equity & Community Medicine curricula give a range of both high-level and hands-on experiences. Dr. Brothers is the Chair of Sutter Medical Group’s Race, Equity, Diversity & Inclusion (REDI) Taskforce. Residents can spend additional elective time in an advocacy rotation which could include accompanying lobbyists to the Capitol, attending County Board of Supervisor meetings, participating in Health Action networks, networking with community organizations, and/or writing letters to the editor - there are always a variety of advocacy efforts going on around the Capitol. For instance, at the local government level, Dr. Brothers also serves as the District 2 (Davis) Board Member of the Yolo County Community Services Action Board. We also offer a leadership elective to help residents hone skills as physician team leader, as well as for a range of other leadership roles. For example, Dr. Julia Logan (FMRP class of 2008) has held a number of state-wide leadership roles including as an Associate Medical Director at the California Department of Healthcare Services (DHCS).

We are proud of our residents’ consistent engagement in community volunteering activities. Although residency is busy, we ensure there is spare time to volunteer at underserved medical clinics, attend community meetings, and engage in meaningful activities as part of the larger community. We have regular protected afternoons for teambuilding activities, which often are chosen as group activities volunteering throughout local communities. We also partner with many community organizations to collaborate on improving the health of our neighborhoods and addressing social determinants of health and inequities on a more systemic level. Please see other sections and slideshows on our website for more information.
Unless we speak up in our community, our voices will not be heard, and the needs of our patients will not be met. Have you found your voice yet? Maybe we can help!
The Sacramento area is unique in that there are 8 Student Run Clinics (SRCs) where local students and Family Medicine residents can volunteer. Traditionally, the Family Medicine residency programs in the area have been very involved in the student run clinics. As a resident, one finds that, after a short time, he or she can quickly pass on what they have learned to budding medical students. The teaching is valuable to the student and the resident. The patients are so appreciative.
For more information on the local SRCs, please see the UC Davis School of Medicine.
To compare Sacramento’s abundance of SRCs with that of other cities around the country, please see the website for the Society of Student-Run Free Clinics.
We value service to the underserved and disenfranchised populations. Taking care of our local population’s health is not only compassionate, it is a moral imperative.
Many residents have entered our program to continue their quest in helping the underserved. Some residents trained in the rural and urban University of California PRIME programs before residency and have plans to return to their underserved communities.
Residents are introduced to marginalized populations from the start on their inpatient Internal Medicine rotation where many uninsured “no-doc” patients are admitted. A variety of pathologies are learned on this rotation including infectious disease, chronic liver and kidney disease, advanced cancer manifestations, substance abuse, and malnutrition.
Through community rotations, residents can work with underserved populations through the County health services, the Davis Community Clinic, Correctional Medicine, Addiction Medicine, Transgender Medicine, and Street Medicine.
Continuity clinic is the ultimate medical home for many of our underserved patients. Although Sutter Health contracts with many private insurance plans, a significant proportion of our patient population is comprised of Medicaid or indigent Medicare folks. Residents learn early on the importance of addressing multiple problems in a visit, as well as the psychosocial context of the patient, and cost-effective medication management.
Sutter Health has a relationship with WellSpace Health, a local FQHC (federally qualified health center). They specialize in mental health and substance abuse disorders. WellSpace Health has joined forces with our Emergency Department (ED) through the T3 Program (Triage, Transport, and Treat).
Our residents have also mentored local low-income high school students to pursue a career in the health sciences (see our Future Faces of Family Medicine section). Many of us have also volunteered in the local student run clinics (see Student Run Clinics section). Some residents and faculty have also served abroad, but as we all know, you don’t have to go that far to find underserved populations! With so many opportunities and so much community need, one physician makes a difference and many physicians together make an even greater impact.
What will be your calling?
Contact Us
Program Director
Dineen Greer, M.D., MPH
Program Manager
Myndee Tran
Sutter Health Family Medicine Residency Program
1201 Alhambra Blvd., Suite 340
Sacramento, CA 95816
(916) 731-7866
If you would like to correspond with our residents, please send your request to: sutterfmrp@sutterhealth.org
To reach the Alhambra Family Medicine Residency Clinic:
Patient Clinic Appointments: (916) 451-4400
Clinic Fax: (916) 731-7955